How Will The Medicare Part D Benefit Change Under Current Law and Leading Propos
Since 2006, Medicare beneficiaries have had access to prescription drug coverage through Part D, where private plan sponsors contract with Medicare to provide the drug benefit. In recent years, policymakers have expressed concerns about the absence of a hard cap on out-of-pocket spending for Part D enrollees, the significant increase in Medicare spending for enrollees with high drug costs, and the relatively weak financial incentives faced by Part D plan sponsors to control high drug costs. Recent proposals aim to address these concerns, including the Trump Administration’s Fiscal Year 2020 budget, the bipartisan prescription drug bill passed by the Senate Finance Committee, and H.R.3, the prescription drug bill recently announced by Speaker Pelosi (D-CA). This brief describes how the Medicare Part D benefit will change in 2020 under current law and proposed changes that would affect what beneficiaries, plans, manufacturers, and Medicare pay for drug costs under Part D in the future.
How Are Total Drug Costs Under Part D Divided Up?
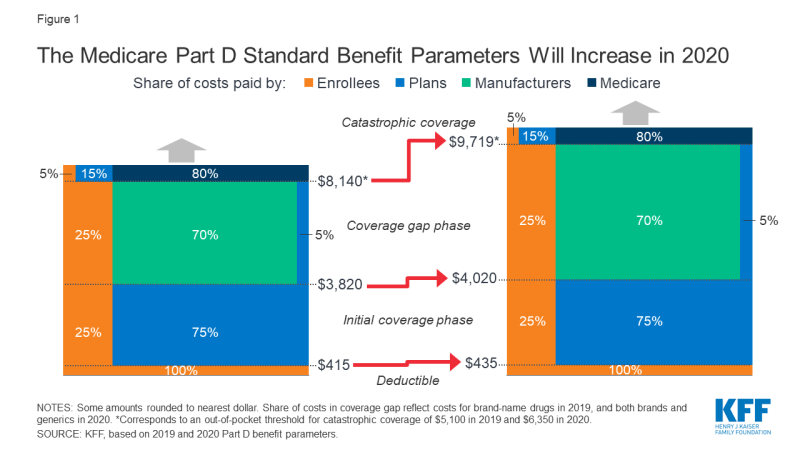
The Medicare Part D standard benefit has different phases where enrollees, Part D plan sponsors, drug manufacturers, and Medicare pay varying shares of total drug costs. These phases include a deductible, an initial coverage phase, a coverage gap phase (once known as the “doughnut hole”), and catastrophic coverage (Figure 1). The allocation of costs in each benefit phase was spelled out in the Medicare Modernization Act of 2003 (the law establishing the Part D program), and has been modified through subsequent legislation.
The Four Medicare Part D Coverage Phases
Medicare Part D includes four main stages: the deductible, initial coverage, coverage gap (also called the “donut hole”), and catastrophic coverage.
Each phase changes how much you pay.
1. Deductible Phase
During the deductible phase, enrollees without Low-Income Subsidies (LIS) pay 100% of their prescription drug costs. Once they meet the deductible, they move into the next stage.
2. Initial Coverage Phase
After meeting the deductible, cost sharing becomes more balanced.
-
Enrollees pay 25% of drug costs
-
Part D plans cover the remaining 75%
This phase continues until total drug spending reaches the initial coverage limit.
3. Coverage Gap (Donut Hole)
After hitting the initial coverage limit, enrollees enter the coverage gap.
Here’s how costs break down:
For brand-name drugs:
-
Enrollees pay 25%
-
Part D plans pay 5%
-
Drug manufacturers provide a 70% discount
For generic drugs (2019 structure):
-
Enrollees pay 37%
-
Part D plans pay 63%
Importantly, both what you pay and the manufacturer discount count toward reaching catastrophic coverage.
4. Catastrophic Coverage Once your annual out-of-pocket spending crosses the catastrophic threshold:
-
Enrollees pay 5%
-
Part D plans pay 15%
-
Medicare pays 80%
This phase offers significant relief for people with very high drug costs.
How the Affordable Care Act Changed the Coverage Gap
Originally, non-LIS enrollees paid 100% of drug costs in the coverage gap.
However, the Affordable Care Act gradually closed this gap by 2020. It reduced enrollee costs to 25%, required manufacturers to discount brand-name drugs by 50%, and increased plan responsibility.
Later, the Bipartisan Budget Act of 2018 accelerated these changes. Starting in 2019:
-
Beneficiary coinsurance for brand drugs dropped from 30% to 25%
-
Manufacturer discounts increased from 50% to 70%
-
Plan responsibility for brand drugs fell from 25% to just 5%
As a result, today’s Part D structure places more responsibility on drug makers while easing the burden on beneficiaries.
What’s Changing in Part D for 2020 Under Current Law?
Several Medicare Part D costs increased in 2020. These changes affect deductibles, out-of-pocket limits, and how much enrollees, plans, and drug manufacturers pay.
Let’s break it down.
Higher Out-of-Pocket Costs Before Catastrophic Coverage
In 2020, Part D enrollees must spend more out of pocket before they qualify for catastrophic coverage.
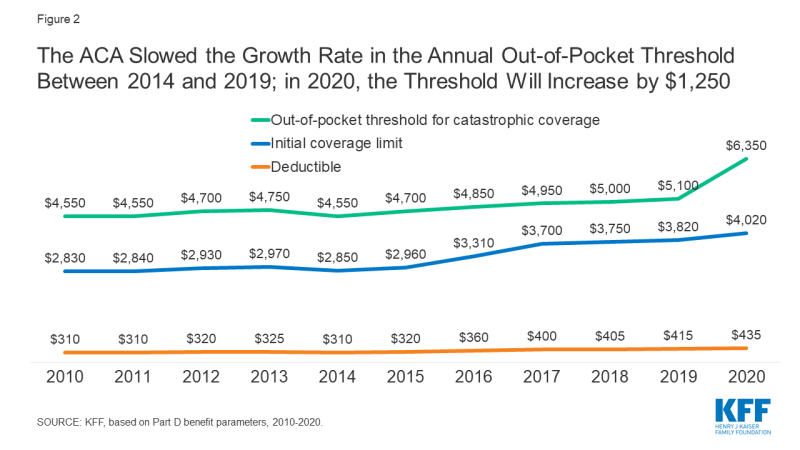
The threshold jumped by $1,250, rising from $5,100 in 2019 to $6,350 in 2020. This increase happened because a temporary Affordable Care Act provision expired. That rule had slowed cost growth between 2014 and 2019. Starting in 2020, the calculation returned to pre-ACA levels.
As a result, many beneficiaries now pay more before receiving catastrophic coverage.
Figure 2: The ACA Slowed the Growth Rate in the Annual Out-of-Pocket Threshold Between 2014 and 2019; in 2020, the Threshold Will Increase by $1,250
Higher Out-of-Pocket Costs Before Catastrophic Coverage
In 2020, Part D enrollees must spend more out of pocket before they qualify for catastrophic coverage.
The threshold jumped by $1,250, rising from $5,100 in 2019 to $6,350 in 2020. This increase happened because a temporary Affordable Care Act provision expired. That rule had slowed cost growth between 2014 and 2019. Starting in 2020, the calculation returned to pre-ACA levels.
As a result, many beneficiaries now pay more before receiving catastrophic coverage.
Deductible and Initial Coverage Limits Also Increased
Part D enrollees also face higher costs in earlier coverage stages.
- The standard deductible rose from $415 to $435.
-
The initial coverage limit increased from $3,820 to $4,020.
During the coverage gap, beneficiaries now pay 25% for both brand-name and generic drugs. Plans cover the remaining 75% of generic drug costs.
This change officially closes the Part D “donut hole” in 2020.
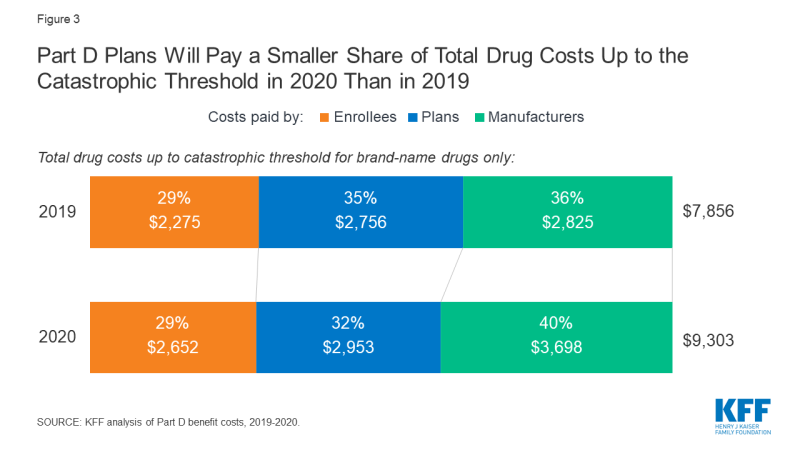
Figure 3: Part D Plans Will Pay a Smaller Share of Total Drug Costs Up to the Catastrophic Threshold in 2020 Than in 2019
What This Means for Enrollees Using Brand-Name Drugs
Non-LIS enrollees who use only brand-name drugs and reach catastrophic coverage will pay nearly $400 more in 2020.
Their annual out-of-pocket costs rise from $2,275 in 2019 to $2,652 in 2020. That increase includes:
-
$20 more for the deductible
-
$45 more during initial coverage
-
$312 more in the coverage gap
Enrollees who use only generic drugs must cover the entire $1,250 increase themselves.
How the Changes Affect Plans and Drug Manufacturers
Part D plans now pay a smaller share of total drug costs for brand-only users.
-
Plans cover 32% in 2020, down from 35% in 2019.
-
Their total dollar increase equals about $197 per enrollee.
Drug manufacturers shoulder more responsibility:
-
Their share rises to 40% in 2020, up from 36% in 2019.
-
They absorb an average increase of $873 per enrollee due to the required 70% discount on brand-name drugs in the coverage gap.
Could These Changes Lower Premiums?
Plans now pay 5% of drug costs for a longer period during the coverage gap, which increases their liability in that phase.
However, fewer enrollees are expected to reach catastrophic coverage in 2020. Since plans pay 15% of costs in that stage, overall plan expenses may decline.
Because most beneficiaries never enter the coverage gap, total plan costs could fall on net — which may help keep premiums lower.
How Many Part D Enrollees Could Be Affected By These Changes?
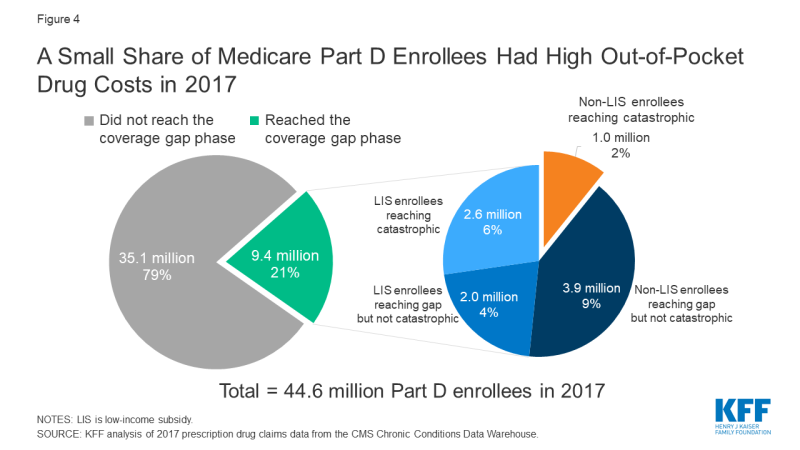
While there are no precise estimates of the number of Part D enrollees who will be affected by the increase in the out-of-pocket threshold for 2020, the increase will directly affect Part D enrollees with very high out-of-pocket drug costs. In 2017 (the most current year of Part D claims data available), 4.9 million non-LIS enrollees reached the coverage gap phase; of that total, 1 million non-LIS enrollees had out-of-pocket drug costs that exceeded the catastrophic threshold (Figure 4). Had the threshold been higher in 2017, fewer than 1 million enrollees would have qualified for catastrophic coverage that year. This means that a larger number of enrollees would have remained in the coverage gap in 2017, where they pay a larger share of their total costs than in the catastrophic phase.
Proposed Changes to the Medicare Part D Benefit Design
Lawmakers continue to push reforms to fix two major issues in Medicare Part D: rising catastrophic spending and the lack of a hard cap on out-of-pocket drug costs. As a result, several proposals aim to limit what beneficiaries pay while shifting more financial responsibility to Part D plans and drug manufacturers.
Let’s look at the key proposals.
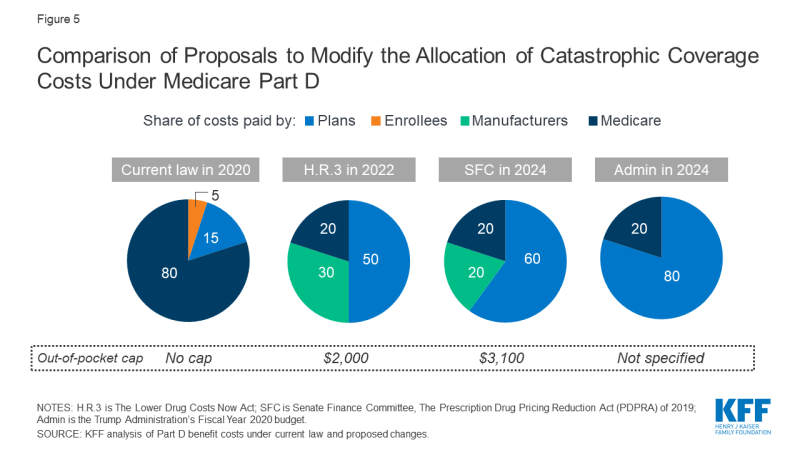
Figure 5: Comparison of Proposals to Modify the Allocation of Catastrophic Coverage Costs Under Medicare Part D
Trump Administration FY 2020 Proposal
In its FY 2020 budget, the Trump Administration proposed adding an out-of-pocket spending limit to Medicare Part D.
Under this plan, beneficiary coinsurance during the catastrophic phase would gradually drop from 5% to 0% over four years, starting in 2020.
At the same time, Part D plans would take on a much larger share of catastrophic costs. Their responsibility would rise from 15% to 80%. Meanwhile, Medicare’s share would fall sharply from 80% to 20%.
The goal: reduce taxpayer burden while encouraging plans to control drug prices.
Senate Finance Committee Proposal (July 2019)
In July 2019, the Senate Finance Committee approved legislation that included a $3,100 annual cap on out-of-pocket drug spending, scheduled to begin in 2022.
The proposal also restructures cost-sharing above the catastrophic threshold:
-
Medicare’s share would drop from 80% to 20%
-
Part D plans’ share would increase from 15% to 60%
-
Drug manufacturers would cover 20% of costs
This plan would also eliminate manufacturer discounts in the coverage gap. Instead, manufacturers would contribute directly to catastrophic costs.
Lawmakers designed these changes to roll out gradually between 2022 and 2024.
House Proposal Led by Speaker Nancy Pelosi (September 2019)
In September 2019, Speaker Nancy Pelosi introduced legislation to further reshape the Part D benefit.
This proposal sets a hard $2,000 cap on beneficiary out-of-pocket spending.
For costs above the catastrophic threshold:
-
Medicare would pay 20%
-
Part D plans would pay 50%
-
Drug manufacturers would pay 30%
The House plan also eliminates the coverage gap entirely. In addition, it changes the initial coverage phase by requiring manufacturers to cover 10% of drug costs.
If enacted, these changes would take effect in 2022.
Conclusion
In the absence of a change in law, Medicare Part D enrollees can expect to face an increase in their out-of-pocket drug costs in 2020. Costs for Part D plan sponsors and drug manufacturers will also increase in dollar terms—but in terms of the share of total drug costs up to the catastrophic threshold, Part D plan sponsors will pay a smaller share in 2020 than in 2019, while manufacturers will pay a larger share. These changes are also likely to affect Part D premiums in 2020 and future years.
Proposed changes to the Part D benefit design would help to mitigate out-of-pocket drug cost increases for Medicare beneficiaries, particularly for those with high drug costs who currently face no limit in their annual out-of-pocket expenses, with Part D plan sponsors and drug manufacturers potentially picking up much of the additional cost.